Diabetes and Its Long-term Complications

Retinopathy, neuropathy, and nephropathy are complications of diabetes, which can cause serious problems if left unchecked and untreated. They originate from uncontrolled hyperglycemia or high blood glucose levels, raised blood pressure, and abnormal lipid levels. These are indications of progression of diabetes to metabolic syndrome. All patients of diabetes should look for early signs and warnings of these long-term complications to avoid severe and irreversible damage.
Diabetic Retinopathy (DR)
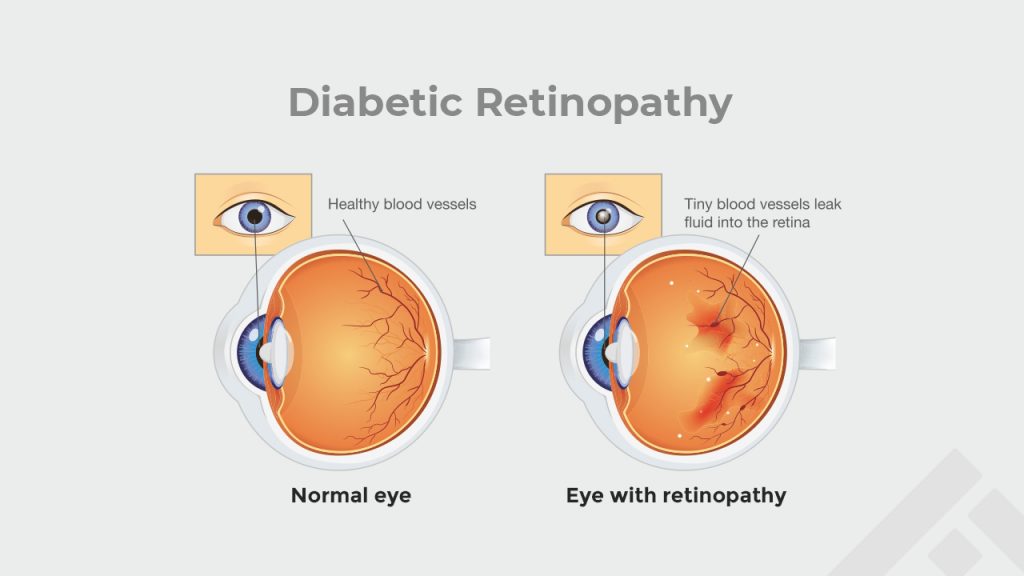
Diabetes affects all parts of your eye and is a leading cause of loss of vision in patients with diabetes mellitus. It can cause damage to blood vessels of the retina, which is a light sensitive tissue at the back of the eye.
1. Prolonged high blood sugar levels can lead to blockage of the blood vessels of the retina. To compensate for this, new blood vessels form. These may not develop properly, leading to leakage of blood into the area and thus affecting vision.
2. The damaged blood vessels can also lead to leakage of fluid into the part of the retina responsible for clear central vision (the macula), which may cause blurred vision.
The loss of vision is mild at first, but progresses to severe loss if left unchecked. Eighty percent of diabetes mellitus patients, who have the condition for more than 20 years, develop diabetic retinopathy.
Symptoms
DR usually affects both eyes. It might be hard to detect initially. However, with the progression of the condition, you may observe symptoms like:
- Seeing dark spots or strings
- Blurry vision
- Fluctuating vision, where sometimes you see clearly and sometimes blurry
- Not being able to differentiate between colours properly
- Empty or dark areas in your vision
- Difficulty seeing in dark
- Complete loss of vision in later stages
Treatment
Management of DR requires a targeted approach aimed at treating the damaged blood vessels as well as stopping the progression of retinal degeneration.
Prevention is the first step. Once a diagnosis of diabetes has been confirmed, you should at once consult an ophthalmologist to screen for DR. Thereafter, a yearly checkup is recommended.
A strict control of blood glucose levels and blood pressure is key to preventing DR. Vision loss, which has already occurred, is irreversible
Treatments such as injections of medicines inside the eye, laser therapy, and surgery are available in case retinopathy does occur. However, results of these treatments are variable and effective only for preventing further loss of vision and not reversing damage.
Also read: Type 2 Diabetes: Causes, Diagnosis and Treatment
Diabetic Neuropathy (DN)
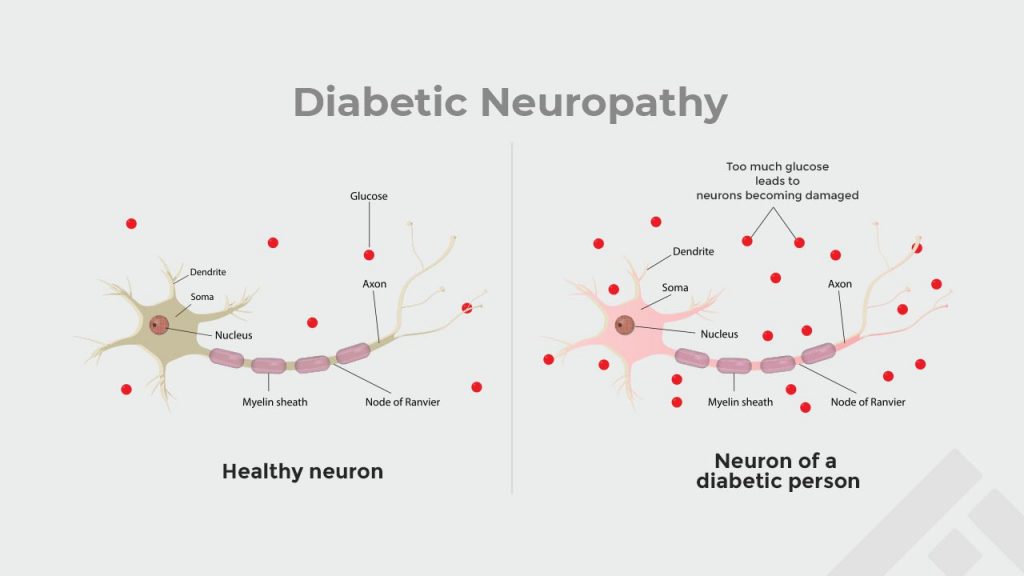
Diabetic neuropathy is a condition that affects the nerves as a result of oxidative damage caused by high blood sugar levels in diabetes. The free radicals formed by degradation of glucose damage the nerves and the blood vessels supplying them. Around 50% of patients with diabetes are affected by some or other form of neuropathy, which is a cause of considerable morbidity.
Symptoms
The symptoms of DN are vast. They can range from pain and tingling in your limbs to problems in the digestive system, blood vessels, urinary tract, and heart, depending on which nerves are affected.
There are four basic types of DN:
1. Peripheral Neuropathy — Diabetic Foot
Peripheral neuropathy affects the upper and lower limbs, causing pain and/ or loss of sensation.
You may experience:
- Tingling or burning sensation in feet
- Sharp pains or cramps
- Numbness or reduced sensations of pain, or temperature changes
- Serious foot problems, like ulcers, infections, and bone and joint pain
This condition is dangerous because any injury or infection on the foot goes unnoticed due to loss of pain sensation. This may progress to a bigger ulceration and cause damage and death of the tissue, which is commonly known as gangrene. In severe cases, the part(s) that develop gangrene may require amputation.
2. Autonomic Neuropathy
This type affects your heart and blood vessels, digestive system, urinary tract, sex organs, and eyes.
You may experience:
- Bladder or bowel problems
- Nausea, loss of appetite, and vomiting due to slow emptying of your stomach
- The way your eyes adjust from light to darkness is altered
- Reduced sexual response
3. Proximal Neuropathy
This type causes pain in thighs, hips, buttocks, or legs predominantly on the side of the body.
You may experience:
- Eventual weakening and shrinking of the thigh muscles
- Difficulty getting up from a sitting position
- Severe stomach pain
4. Focal Neuropathy
Focal neuropathy affects selective areas, including eyes, facial and ear muscles, chest, abdomen, and lower limbs.
You may experience:
- Difficulty focusing or double vision
- Pain behind one eye
- Paralysis on one side of your face
- Numbness in your hand, except your little finger
- Weakness in your hand, so much so that it may cause you to drop things
Treatment
Strict control of blood glucose is required for preventing the occurrence of DN in the first place. Care of feet comes next. It is advisable to follow appropriate foot care as soon as the diagnosis of diabetes is confirmed. This is done to ensure early detection and treatment of injuries, which may otherwise progress to the gangrene stage.
The American Diabetes Association recommends the following for foot care on a regular basis:
1. Check your feet every day. If you no longer feel pain in your feet, you might not notice a foot injury. Look carefully for them. Use a mirror to see the bottom of your feet. Use your hands to feel for hot or cold spots, bumps, or dry skin. Look for sores, cuts, or breaks in the skin. Also check for corns, calluses, blisters, red areas, swelling, ingrown toenails, and toenail infections. If it’s hard for you to see or reach your feet, get help from a family member or foot doctor.
2. If your feet are dry, use a lotion on your skin but not between your toes. Wear shoes and socks that fit well and wear them all the time. Use warm water to wash your feet, and dry them carefully afterward.
3. Consult your physician and use special shoes if needed.
4. Be careful with exercising. Some physical activities are not safe for people with neuropathy. Talk with a diabetes clinical exercise expert who can guide you.
Diabetic Nephropathy — Chronic Kidney Disease
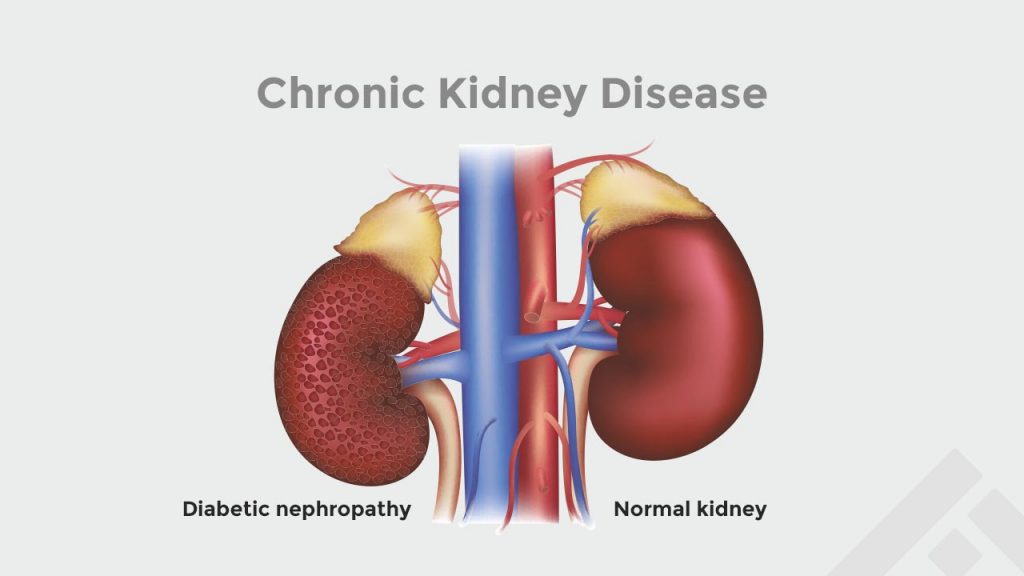
Around 20%-50% of individuals with diabetes ultimately develop Chronic Kidney Disease (CKD) or diabetic nephropathy, commonly called diabetic kidney disorder
It arises as a complication of mainly type 1 and type 2 diabetes. High blood sugar levels affect the primary function of the kidney by putting stress on the filtration system. It leads to leakage of large amounts of protein and salt in urine. As a result, the body suffers from metabolic disorders, changes in pH of body fluids, and multiple organ damages.
Symptoms
- Swelling of feet, hands and ankles (edema) during initial stages, which later progresses to the entire body
- Increased frequency of urination
- Worsening of blood pressure control
- Difficulty concentrating or focusing
- Itching
- Weakness, fatigue
- Loss of sleep
- Upset stomach, poor appetite
Treatment
Strict control of blood sugar is the key to preventing progression to diabetic nephropathy. Levels of blood sugar, Hemoglobin A1C (HbA1c) should be checked regularly or as advised by a physician. Kidney function tests form part of follow-up in all diabetic patients.
Advice of a qualified dietician should be sought in case diabetic nephropathy has already set in. The diet is individualized based on glucose levels, stage of kidney disease, and presence of other diseases along with diabetes.
Initial treatment of diabetic nephropathy is aimed at controlling blood pressure, increasing function of the kidney, and reducing the loss of protein and salt from the body. In later stages of kidney disease, patients may require lifelong dialysis, which is a time-consuming and expensive procedure and requires frequent visits (3 to 4 times per week) to the hospital.
How to manage diabetes
1. Strict control of blood sugar is the cornerstone of diabetes management in the long term and the best way of avoiding life-threatening complications.
2. Once diabetes has been diagnosed, regular tests for blood glucose and HbA1c are a must for monitoring the disease.
3. Eye check-up by an ophthalmologist upon diagnosis, and thereafter on a yearly basis is helpful in early detection and treatment of eye complications associated with diabetes.
4. Foot care is of utmost importance in patients of diabetes since diabetic neuropathy can cause damage to nerves of feet and lead to gangrene of the foot. The only treatment once gangrene has set in is amputation of the limb.
5. Kidney disease is a severe complication of diabetes, which affects up to 50% of patients. Regular tests, lifestyle changes and strict diet control go a long way in preventing damage to the nephrons and deterioration of the disease.
References
1. Kertes PJ, Johnson TM. Evidence-Based Eye Care. Philadelphia, PA: Lippincott Williams & Wilkins (LWW), 2013.
2. Diabetes. American Diabetes Association. https://www.diabetes.org/diabetes/complications (accessed Mar 1, 2021).
3. Neuropathy. American Diabetes Association. https://www.diabetes.org/diabetes/complications/neuropathy/steps-prevent-or-delay-nerve-damage (accessed Mar 1, 2021).
4. Varghese RT, Jialal I. Diabetic Nephropathy. Treasure Island, FL: StatPearls Publishing.
5. Schreiber AK, Nones CF, Reis RC, et al. Diabetic Neuropathic Pain: Physiopathology and Treatment. World J Diabetes 2015; 6: 432–44.
6. Wong MYZ, Man REK, Fenwick EK, et al. Dietary Intake and Diabetic Retinopathy: A Systematic Review. PLoS One 2018; 13: e0186582.
7. Wang W, Lo ACY. Diabetic Retinopathy: Pathophysiology and Treatments. Int J Mol Sci 2018; 19: 1816.