How to Stay Consistent in Your Training

Several studies have attempted to demonstrate a dose-response relationship between physical activity levels and mortality rates. The relationship between the two appears to be inverse and curvilinear, where if the dose of exercise (particularly moderate to vigorous physical activity levels) increases, there are corresponding decreases in mortality.
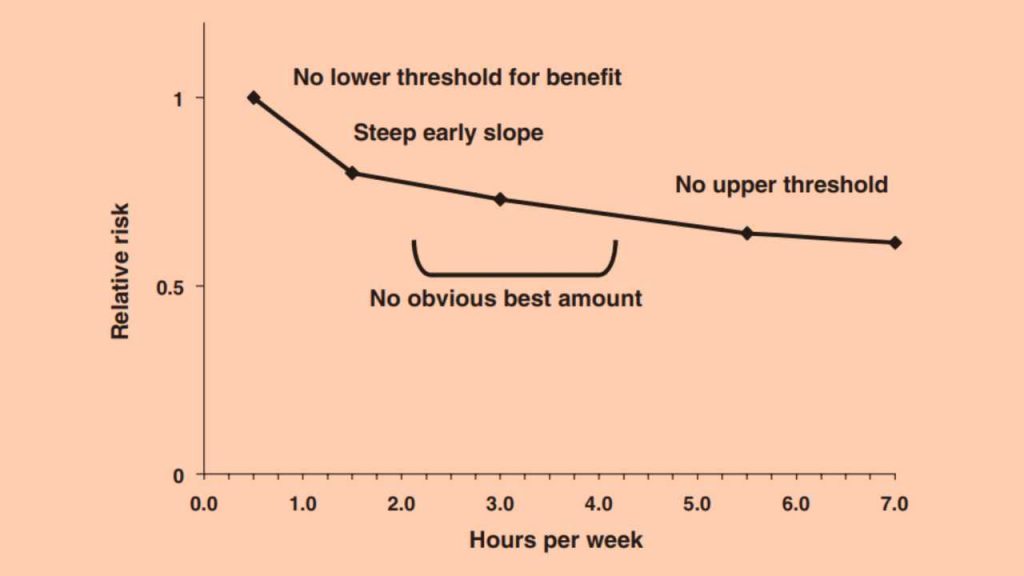
Specifically, ≥6hours of moderate to vigorous physical activity levels performed per week sees a nearly 40% reduction in mortality risk (Figure 1). However, most of us do not participate in minimum recommended weekly physical activity doses. In India, a large population study of 14,227 individuals established that nearly half of the population were inactive, which translates to approximately 392 million inactive individuals across all of India.
Additionally, among those who reported recreational physical activity, the time spent in moderate to vigorous intensity activity overall was <20 mins/day, with many of these activities being performed within the workplace.
Altogether, one thing remains quite clear based on the population-based evidence, and that is that people often fail to adhere to long-term training/ physical activity programs. Social and family constructs, support network, lifestyle changes, age/ ageing, geographical barriers, accessibility, transportation, and many other factors play significant roles in whether a person undertakes, and maintains, physical training.
As such, particularly with the recent global outbreak of the novel SARS-COVID-19 virus, it is becoming exceedingly difficult to maintain healthy fitness habits. Let us explore what barriers might prevent exercise participants, and/ or exercise adherence patterns, along with some handy tips on how to overcome these common barriers and stay consistent in training.
What causes inconsistency in training?
Perceived barriers and other unique issues: One study undertaken over 3.2 years and tracking physical activity levels of 1,076 participants showed that top weight loss barriers included problems with self-monitoring (58%), social cues (58%), holidays (54%), low activity (48%), and internal cues (ie, thoughts/ mood state) (44%). In addition, top physical activity barriers included holidays (51%), poor time management (50%), internal cues (30%), illness (29%), and lack of motivation (26%).
Another review synthesising information across 11 population-based studies found that among South Asian older adults (ie, from across Afghanistan, Pakistan, Indian, Nepalese, Bhutan, Bangladesh, the Maldives, and Sri Lankan) there were several unique issues preventing physical activity participation.
- Language: An inability to understand English or possibly being illiterate in their own language can make some South Asian older adults reliant on family members for information about health behaviours.
- Prevention: Unfamiliarity with the concept of accessing health information for preventive reasons rather than seeking it for advice on how to treat a condition following onset.
- Group norms: Peer mentors facilitating exercise opportunities or a sense of it being inappropriate for women to be physically active.
- Fate: Feeling that health is shaped by a higher force, so individuals do not believe they are able to prevent disease through behaviours such as exercising.
- Cultural sensitivity: A lack of single sex exercise classes with same sex instructors.
- Collectivist attitudes: Taking time to look after oneself (eg, exercising) running counter to a collectivist view of acting for the family and the wider community.
Injury setbacks: Besides the barriers listed above concerning physical activity in the general population, other setbacks, like injury, may also disturb long-term training adherence. Injuries can result in poor health-related quality of life outcomes including drops in self-efficacy, motivation losses, increases in anxiety, and depression. A loss in confidence may discourage individuals from returning to physical activity following an injury setback, which is of course highly dependent on the nature of the injury and recovery time. Long-term injuries such as ACL ruptures, which typically take 12 months to fully recover from, can result in significant mental health declines and lead to poor physical activity adherence rates post-recovery.
COVID lockdowns: A worrying trend currently among general populations is the flipped nature of physical activity versus sedentary behaviour time (ie, television viewing, periods of inactivity etc.) during COVID-19-enforced lockdowns. A recent systematic review of 66 research articles, and a total of 86,981 participants across the world, showed a broad trend towards people decreasing physical activity levels and increasing sedentary behaviours while in lockdown. It was noted that due to the paradigm shift between physical activity and sedentary behaviours, both physical and mental health were negatively impacted.
How to manage training inconsistencies
Generally, it is recommended that several strategies (often unique to the individual) be implemented to increase physical activity and decrease sedentary behaviours. While these strategies are broad, some of the following may prove helpful in avoiding training inconsistencies (Table 1).
| Increase physical activity adherence rates | Decrease sedentary behaviours |
| Bodyweight home-workouts can be performed quickly (within 25-30mins) and with high intensities, which is key to optimising health outcomes. | Use a standing desk while working from home. |
| Using online exercise classes — a lot of exercise classes are now available online, where you can listen to the instructor and perform the movements from home. | Take regular breaks from sitting, every 30 mins. |
| Change the mode of training — walking, running and/or cycling outdoors can be great alternatives to indoor circuit training. | Avoid spending excessive time on your phone (social media). Aim to set an upper limit on screen time, like 1-2 hrs per day maximum. |
| Invest in indoor aerobic equipment such as stationary cycles, rowers, treadmills etc. | |
| Look to engage in community-driven (social) exercise classes or sporting events. | |
| Ask your family relatives to be involved in the physical activity planning — they can help you to stay motivated and on track. |
Novel training ideas can also add significant value to a workout plan, particularly if the training does not feel like training. For instance, active video gaming strategies (also called exergaming) can be a great way to introduce daily incidental physical activity while having fun and playing games. Evidence is growing regarding the use of exergames in maintaining physical activity levels from within the home setting, particularly for adults and older adults (>65 years).
Also read: How to Exercise Regularly and Stay Motivated
In addition, other tips to stay on track with training include:
1. Use positive reward strategies.
2. Set small, easily achievable goals and be sure to tick them off as you go along.
3. Use reminder systems — setting alarms on your phone, computer monitor, smart watch etc. can prompt you to get moving.
4. Do activities that you enjoy. If you enjoy the activity, you are much more likely to adhere to the exercise program long term.
5. Use the Fitpage app to track your progress and plan your daily workout routines.
6. Many of us avoid exercise because we perceive it to be too difficult and that we do not have enough time in the day to fit it in. Doing 15mins of mindfulness training in the morning can put you into a positive frame of mind and can help you plan your day to ensure you fit in time to exercise.
7. Train with a friend/training partner. They will help keep you motivated.
8. Invest in a personal trainer. Despite the cost, personal trainers will plan the daily exercise routine for you and will keep you motivated.
9. Record your training/ fitness results in a diary or on your laptop/ iPad. This will help you when you plan your goals.
References
1. Venditti, E. M., Wylie-Rosett, J., Delahanty, L. M., Mele, L., Hoskin, M. A., & Edelstein, S. L. (2014). Short and long-term lifestyle coaching approaches used to address diverse participant barriers to weight loss and physical activity adherence. International Journal of Behavioral Nutrition and Physical Activity, 11(1), 1-12.
2. Stockwell, S., Trott, M., Tully, M., Shin, J., Barnett, Y., Butler, L., … & Smith, L. (2021). Changes in physical activity and sedentary behaviours from before to during the COVID-19 pandemic lockdown: a systematic review. BMJ Open Sport & Exercise Medicine, 7(1), e000960.
3. Horne, M., & Tierney, S. (2012). What are the barriers and facilitators to exercise and physical activity uptake and adherence among South Asian older adults: a systematic review of qualitative studies. Preventive medicine, 55(4), 276-284.
4. Powell, K. E., Paluch, A. E., & Blair, S. N. (2011). Physical activity for health: What kind? How much? How intense? On top of what?. Annual review of public health, 32, 349-365.
5. Anjana, R. M., Pradeepa, R., Das, A. K., Deepa, M., Bhansali, A., Joshi, S. R., … & Shukla, D. K. (2014). Physical activity and inactivity patterns in India–results from the ICMR-INDIAB study (Phase-1)[ICMR-INDIAB-5]. International Journal of Behavioral Nutrition and Physical Activity, 11(1), 1-11.
6. Ochiai, S., Hagino, T., Tonotsuka, H., & Haro, H. (2011). Prospective analysis of health-related quality of life and clinical evaluations in patients with anterior cruciate ligament injury undergoing reconstruction. Archives of orthopaedic and trauma surgery, 131(8), 1091-1094.
7. Rüth, M., & Kaspar, K. (2021). Educational and Social Exergaming: A Perspective on Physical, Social, and Educational Benefits and Pitfalls of Exergaming at Home During the COVID-19 Pandemic and Afterwards. Frontiers in psychology, 12.