Osteoporosis: Causes, Symptoms and How to Manage It

Osteoporosis, which literally translates into “porous bone”, is a condition where the bones in your body become less dense. It makes the way for fractures or other bone injuries even on minor falls. Once your bones become brittle, it becomes difficult to prevent fractures.
Since age is a risk factor, older adults usually suffer from osteoporosis, but it can occur at any age. Postmenopausal women are also at greater risk because of low estrogen levels. Along with hormonal imbalances, family history, eating disorders and low calcium intake, underlying medical conditions, lifestyle choices too, play a role in developing osteoporosis. But you can lower the risks by eating and living healthy, exercising, and maintaining your body weight.
How does osteoporosis occur?
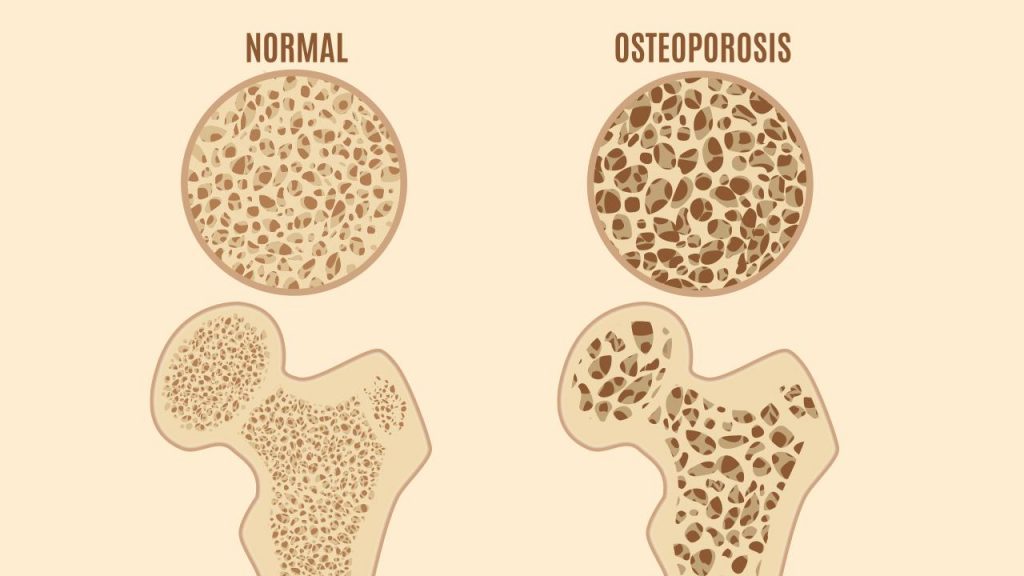
Bone is made up of organic (predominantly protein) and inorganic (mineral) components. The bone tissue undergoes a continuous natural process of formation and breakdown throughout our lifetime. During bone formation, calcium and other minerals get packed into the tissue and during the breakdown, they are removed. The process of old bone tissue being replaced by healthy ones is called remodeling.
Till approximately the age of 30, the replacement happens at a pretty quick rate. As you start aging, the process slows down. The degeneration and removal of minerals from bone leads to low bone density, making them brittle. The vertebrae or the spinal column, hip, and wrists are most susceptible to fractures caused by osteoporosis.
Early and late stages
A lot of the time, the terms osteopenia and osteoporosis are used interchangeably. They aren’t the same, however. Both are varying degrees of bone loss, which is measured by bone mineral density (BMD), which is the amount of mineral per unit area of bone. BMD is measured by a scoring system — the T-score — after analyzing x-rays of various bones of the body.
In osteopenia, the T-score is less than what it should be in a normal person but is not low enough to be diagnosed as osteoporosis. During osteopenia, fractures don’t happen that easily. But if left untreated, osteopenia can slowly progress to osteoporosis. A T-score of -2.5 or lower indicates osteoporosis.
Symptoms of osteoporosis
There are no obvious symptoms during the early stages of bone loss. During advanced osteoporosis, some common symptoms are:
- Severe aches and pains around joints and backaches
- Loss of height over time due to loss of bone tissue in vertebrae
- Kyphosis (hunched posture)
- Sudden fractures of the hip joint, wrist joint, or vertebrae without any obvious or notable trauma
What are some of the risk factors
Here are some of the factors that increase your risk of osteoporosis.
Family history: Having a family history of osteoporosis may increase your chances of developing it.
Age: Women over age 55 and men over age 65 are commonly affected by osteoporosis.
Sex: Women are at a higher risk for osteoporosis, especially after menopause. The hormone estrogen helps in protecting the body from bone loss. However, after menopause, estrogen production is greatly reduced. Any condition that reduces estrogen levels can pose a risk for bone loss.
Hormones: Conditions that may cause low estrogen levels in women and testosterone in men may compromise bone health. Certain medicines, surgeries, and hormonal imbalance in the body caused by problems in the thyroid and parathyroid glands can increase your risk of osteoporosis. Stress-induced increase in levels of cortisol can also have a negative effect on bone health.
Nutrient deficiency: Having a prolonged deficiency of vitamin D and calcium can create problems.
Physical inactivity: People who lead a sedentary lifestyle or those who are bedridden are more vulnerable.
Bodyweight and structure: Individuals with a slimmer or petite frame tend to be at higher risk for bone loss than individuals with bigger frames.
Smoking: Smoking may cause impaired calcium absorption from the diet.
Alcohol: Consumption of excess alcohol is found to be a risk factor for osteoporosis.
Others: Long-term use of certain medications like those used for the treatment of seizures, certain anti-estrogen medications, or anticancer drugs can cause an imbalance in the formation and resorption of the bone, thus leading to osteoporosis.
Management of osteoporosis
Severe cases of osteoporosis may require intensive treatment. But primary treatment is generally aimed at stopping further bone loss. Check out a few things you can do.
Diet: Having a healthy diet rich in fruits and vegetables and foods rich in calcium and vitamin D can reduce risks. A soya-rich diet is recommended for women by experts since soya is rich in estrogen. It’s believed soya helps balance the bone loss that occurs around menopause.
Lifestyle: Lifestyle should be modified to incorporate adequate physical activities.
Correcting underlying conditions: It is important to understand that if there is an underlying health condition, such as a hormone deficiency that is causing osteoporosis, you would need to address it medically.
Medications: A few medicines are available for the treatment of osteoporosis. However, most are not tolerated very well by older people due to high incidences of side-effects. Medications should be taken only after consulting a qualified physician.
Changing ongoing medications: If you are on any medication that contributes to osteoporosis, your physician may suggest alternatives.
How can you keep your bones healthy?
A balanced diet and a healthy lifestyle can help you maintain good bone health. Here are some tips on how to go about it.
Calcium: Foods like milk and other dairy products, soya beans, tofu, green vegetables like broccoli and cabbage are good sources of calcium. The main calcium intake is from dairy foods. Vegans can consume calcium-fortified foods (foods to which calcium is added), soya, sesame seeds, pulses, dried raisins, figs, and apricots.
Vitamin D: Some vitamin D food sources are fatty fish such as salmon and mackerel, eggs, and vitamin D-fortified foods like cereals. Vegans can consume vitamin D-fortified foods and dietary supplements, as directed by a physician. But it is not possible to get the required quantities from diet alone. One of the best natural sources is the sun. It is suggested that exposing the face, arms, hands, and legs to the sun, without the application of sunscreen, for five to 30 minutes, especially between 10am and 4pm every day or at least twice a week can help the body produce sufficient vitamin D.
Lifestyle: An active lifestyle plays a significant role in maintaining healthy bones. Regular physical exercise not only helps in improving muscle strength but also helps in maintaining bone health. You must engage in at least 30 minutes of physical activity daily. Research suggests that activities involving varied, mild to moderate spinal movements can help preserve the health and strength of the spine. Resistance exercises like weight lifting can improve bone health, as can weight-bearing exercises (in which your bones support your body weight) such as hiking, walking, running, stair climbing, and dancing. If you have any underlying condition or risk factors for osteoporosis, consult a physician before engaging in strenuous activities.
Practicing yoga is recommended for maintaining healthy bones. Weight-bearing yoga asanas and poses that provide mild spinal flexion and extension can be helpful. It is advisable to perform such exercises under the guidance and supervision of an expert as incorrect posture and technique can lead to injuries.
It is recommended to avoid the consumption of excess alcohol and cigarette smoking.
When you are young, maintaining bone health is easy. But as you grow older, osteoporosis can easily compromise the quality of your life, even restricting simple activities like bending and lifting. Start taking precautions early to avoid broken bones in the long run.
References
1. Osteoporosis. Cleveland Clinic. https://my.clevelandclinic.org/health/diseases/4443-osteoporosis (accessed Feb 7, 2021).
2. Osteoporosis. National Institute on Aging. https://www.nia.nih.gov/health/osteoporosis (accessed Feb 7, 2021).
3. Food for Healthy Bones. NHS. https://www.nhs.uk/live-well/healthy-body/food-for-strong-bones/ (accessed Feb 7, 2021).
4. Exercise for Your Bone Health. NIH Osteoporosis and Related Bone Diseases National Resource Center. https://www.bones.nih.gov/health-info/bone/bone-health/exercise/exercise-your-bone-health (accessed Feb 7, 2021).
5. Smith E, Boser A. Yoga. Vertebral Fractures, and Osteoporosis: research and recommendations. Int J Yoga Therap 2013; 23: 17–23.
6. Osteoporosis Overview. NIH Osteoporosis and Related Bone Diseases National Resource Center. https://www.bones.nih.gov/health-info/bone/osteoporosis/overview (accessed Feb 7, 2021).
7. Quinn E. The Link Between Exercise and Healthy Bones. Verywell Fit 2019; published online Aug 20. https://www.verywellfit.com/bone-density-and-exercise-3120770 (accessed Feb 7, 2021).
8. Manske S, Lorincz C, Zernicke R. Bone Health: Part 2, Physical Activity. Sports Health 2009; 1: 341–6.
9. Bone mineral density test: MedlinePlus Medical Encyclopedia. Medlineplus. https://medlineplus.gov/ency/article/007197.htm (accessed Feb 7, 2021).
10. Cannarella R, Barbagallo F, Condorelli RA, et al. Osteoporosis from an Endocrine Perspective: The Role of Hormonal Changes in the Elderly. J Clin Med 2019; 8: 1564.
11. Wacker M, Holick MF. Sunlight and Vitamin D: A global perspective for health. Dermatoendocrinol 2013; 5: 51–108.
12. Zheng X, Lee SK, Chun OK. Soy Isoflavones and Osteoporotic Bone Loss: A Review with an Emphasis on Modulation of Bone Remodeling. J Med Food 2016; 19: 1–14.
13. Vitamin D. National Institute of Health. https://ods.od.nih.gov/factsheets/VitaminD-HealthProfessional/#:~:text=Some%20expert%20bodies%20and%20vitamin,13%2C15%2C30%5D (accessed Mar 09, 2021).